Human papillomavirus (HPV) is a nonenveloped double-stranded DNA virus and member of the Papovaviridae family. HPV has a predilection for differentiating squamous epithelium, where it infects and transforms host cells. HPV-related cellular aberrancies in females are concentrated in the squamocolumnar region of the ectocervix, making this region ideal site for diagnostic sampling. Although over 100 strands of HPV have been identified, 35 have been shown to infect the genital epithelium.
Reference ranges, based on the test, are listed below.
Results show the ratio of the specimen reactivity to the positive control mean. A result is considered to be positive if its reactivity is at least that of the positive control. [1, 2]
Amplified DNA from cells harboring human papillomavirus are used as positive controls. Tested samples are compared to the positive controls to determine positivity. [3]
Several different modalities exist for the laboratory diagnosis of genital HPV. The most dominant techniques are polymerase chain reaction (PCR) viral detection and signal amplification DNA-based assays (with Hybrid Capture II and Cervista being signal amplification tests that have been approved by the US Food and Drug Administration [FDA]). [4]
Signal amplification DNA-based assays: The Hybrid Capture II
The sensitivity of Hybrid Capture to detect high-grade (16, 18, 31, 33, 35, 39, 45, 51, 52, 56, 58, 59 and 68) lesions in various studies was 90%, and its specificity in clinical studies is 89%. [5] High-risk probe cocktails have been shown to cross-react with HPV types not included in the probe mix. HC-2 can detect as little as 1 pg/mL of target DNA (5000 genome copies per test). [2]
An RLU/CO ratio of 1.0 or more is considered positive.
RLU/CO ratio less than 1.0 is considered negative or nondetected for the 13 HPV types tested. High-risk HPV DNA sequences are either absent or the HPV solution DNA levels are below the detection limit of the assay.
When testing PreservCyt solution specimens, if the RLU/CO ratio of a specimen is 1.0 or higher and less than 2.5, the test should be repeated. If the initial retest is positive (RLU/CO > 1.0), the specimen is reported as positive, and no further testing is necessary. If the initial retest is negative, then a second retest should be performed. The results of the second retest are considered to be the final result.
Polymerase chain reaction
Sensitivity and specificity are high for PCR at 100% and 99%, respectively. Frequently encountered genital types of HPV can be detected with as few as 10 copies of viral DNA.
Positive test results
If either HPV test shows the presence of a high-risk HPV strain, but the Papanicolaou (Pap) test is normal, then both tests should be repeated in 12 months. If the Pap test is positive, then colposcopy is advised. [6] If both the HPV and Pap test show a positive result for the presence of a high-risk HPV strain, then colposcopy should be performed right away.
Cervical specimens that may be tested with the HC-2 high-risk HPV DNA test include those obtained with the HC-2 high-risk DNA collection devices, biopsies collected in specimen transport medium, and specimens collected using a broom-type collection device and placed in Cytyc Thin Prep Pap test PreservCyt solution.
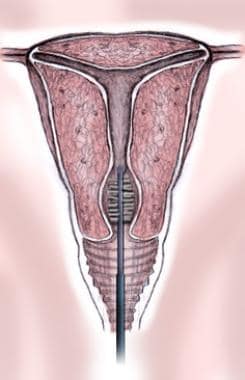
The specimen collected for laboratory diagnosis of genital HPV are exfoliated cells from a female’s cervical junction or a male’s foreskin, balanopreputial sulcus, glans, and navicular fossa of the penis. When using this method of diagnosis, specimen collection must occur prior to acetic acid or iodine use if colposcopy is to follow.
Following placement of a speculum inside the vagina, a conical cytobrush is placed at the cervical os and lightly brushed to ensure attainment of an adequate sample (see image below). (A plastic spatula may also be used instead of a cytobrush and then resuspended into 10-20 mL of liquid cytology medium. This specimen can be held at room temperature for up to 4 weeks.) For male patients, the brush is rubbed against the foreskin, balanopreputial sulcus, glans, and navicular fossa of the penis. [7] The brush is placed into specimen transport medium (STM), which has preservatives to retard bacterial growth and retain the integrity of the DNA.
Following collection, the specimen can be held for up to 2 weeks at room temperature prior to shipping in the STM. If the assay will be performed more than 3 weeks from collection, specimens can be placed at -20°C for up to 3 months prior to testing.

--> empty para to satisfy content model
Freshly collected cervical biopsies 2-5 mm in cross-section may be analyzed by the HC-2 high-risk HPV DNA test. The specimen must be placed immediately into 1 mL of STM and stored frozen at -20°C. Biopsy specimens may be shipped at 2-30°C for overnight delivery to the testing lab and stored at -20°C until processed. Specimens less than 2 mm in cross-section should not be used.
Specimens collected with a broom-type collection device and placed in Cytyc PreservCyt Solution for use in making Cytyc ThinPrep Pap test slides can be used in the HC-2 high-risk HPV DNA test. At least 4 mL of PreservCyt solution must remain for the HC-2 high-risk HPV DNA test. Specimens with less than 4 mL after the Thin Prep Pap test has been prepared may contain insufficient material and could result in a false negative with the HC-2 high-risk HPV DNA test.
Specimens containing the target DNA hybridize with a specific HPV RNA probe cocktail. The RNA-DNA hybrids adhere to the surface of a microplate well coated with antibodies specific for RNA-DNA hybrids. These adherent hybrids are then reacted with alkaline phosphatase–conjugated antibodies specific for the RNA-DNA hybrids and detected with a chemiluminescent substrate. Several alkaline phosphatase molecules are conjugated to each antibody. Signal amplification is the result of multiple conjugated antibodies binding to each adherent hybrid.
Cleavage of the substrate by the bound alkaline phosphatase results in light emittance, which is measured in relative light units (RLUs) on a luminometer. The intensity of the light corresponds with the presence or absence of target DNA in the specimen. An RLU measurement that is equal to or greater than the cutoff value (CO) indicates the presence of high-risk HPV DNA sequences in the specimen, whereas a value less than the cutoff value suggests absence of the specific high-risk HPV DNA sequences tested or levels below the detection limit of the assay. [1]
Human papillomavirus (HPV) is a nonenveloped double-stranded DNA virus and member of the Papovaviridae family. HPV has a predilection for differentiating squamous epithelium, where it infects and transforms host cells. HPV-related cellular aberrancies in females are concentrated in the squamocolumnar region of the ectocervix, making this region ideal site for diagnostic sampling.
Although over 100 strands of HPV have been identified, 35 have been shown to infect the genital epithelium. Genital HPV may present as cutaneous or anogenital warts, skin lesions, or varying degrees of dysplasia and carcinoma. High-risks types most commonly associated with genital warts are strains 6 and 11, whereas strains 16 and 18 are the high-risk types of carcinoma caused by HPV. [8]
HPV is the most common sexually transmitted disease. Infection with HPV most likely occurs when the virus is introduced to an area of skin disruption in the genital tract. Transmission can occur in the absence of active lesions while the disease is in latent phase. [9] The incubation period for HPV diseases range from 1 month to 2 years.
Although many cases of genital HPV clear, persistent HPV may lead to cervical cancer. Manifestations of the disease may be active initially or enter a latent phase where the infected person remains asymptomatic but will still test positive. During the active phase of infection, the squamous epithelial cells proliferate and may become benign tumors known as genital warts and condyloma. HPV has the potential (especially with high-risk types) to integrate into host DNA, disrupting cell management of oncoproteins and tumor-suppressing genes.
Genital HPV types 6 and 11, which cause cutaneous and anogenital warts, can be diagnosed based on clinical inspection. [10] Physical examination and cervical Papanicolaou testing is the primary modality for HPV-related cervical disease diagnosis. The Papanicolaou (Pap) test is the current screening method used to detect HPV. Practioners take a sample of tissue from a woman’s cervical junction, and the sample is examined for the presence of HPV-infected cells. According to current CDC recommendations, females starting at age 21 should receive a Pap test yearly. HPV testing looking to identify the actual virus may be done on females who request the test after age 30 or have an abnormal Pap smear. [11] HPV infections are more likely to resolve in females under the age of 30.
The HC-2 high-risk HPV DNA test is not intended for use as a screening device for Pap in normal women younger than 30 years and should not be used as a substitute for regular Pap screens. Detection of HPV using the HC-2 high-risk HPV DNA test does not differentiate HPV types or infection with more than one type. Furthermore, it cannot evaluate persistence of any one type of HPV. Use of the HC-2 test is indicated to screen patients with atypical squamous cells of undetermined significance (ASC-US) Pap smear results to determine the need for repeat colposcopy, and in women 30 years and older. It can be used as an adjunct to the Pap test to assess the presence/absence of high-risk HPV types, which in conjunction with other patient risk factors, cytology history, and professional guidelines, may be useful in guiding patient management.
Signal amplification DNA-based assays: The Hybrid Capture vs PCR
Signal amplification DNA-based assays amplify detection signals without modifying the initial amounts of sample nucleic acid and can thus detect lower quantities of DNA.
Although 2 sets of RNA probes exist for Hybrid Capture II (HC-2), the probe that detects high-risk strains (16, 18, 31, 33, 35, 39, 45, 51, 52, 56, 58, 59, and 68) is used most often. Genomic amplification and typing using PCR is another method for HPV detection and the criterion standard for HPV research. Frequently encountered genital types of HPV can be detected with as few as 10 copies of viral DNA.
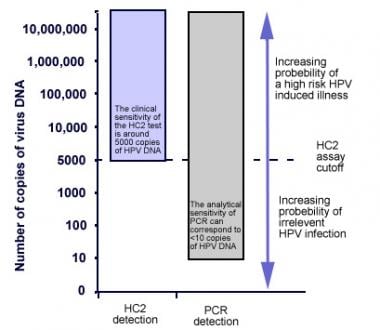
Several studies have shown that while PCR is better at the detection of HPV, rates of high-risk detection are equivalent when using PCR or HC-2 (see the image below). [1]
--> empty para to satisfy content model
Comparison of the hybrid capture 2 HPV DNA-test (HC-2) to the AdvanSure human papillomavirus screening real-time, PCR and the Abbott real-time high-risk HPV PCR assay (Abbott PCR) demonstrate that the AdvanSure HPV screening real-time PCR and the Abbott PCR assay are less sensitive but more specific than the HC-2 assay. [12]
Patients undergoing HPV testing should not be pregnant or be actively menstruating because these situations may disrupt testing.
Due to cross-reactivity in the Hybrid Capture II probes, false-positive results designating high-risk infection may occur if high levels (4 ng/mL or higher) of HPV 6 or HPV 42 are present in the specimen
False-negatives may result from specimens taken from areas with high concentrations of anti-fungal cream, contraceptive jelly, or presence of a douche. [13]
A study by Strang et al in patients who underwent cervical screening for HPV found that at 10-year follow-up, the incidence of high-grade cervical intraepithelial neoplasia (CIN) did not significantly differ with regard to whether the patient had initially been screened with a DNA- or an RNA-based assay. [14]